Breast Health
Breast Cancer Screening in Singapore: All About Mammograms

Breast cancer incidence has nearly tripled in Singapore over the past four decades. According to the Singapore Cancer Registry, more than 9,000 women were diagnosed with breast cancer in Singapore, according to the Singapore Cancer Registry. In Singapore nowadays, one in every thirteen to sixteen women would develop breast cancer during her lifetime.

Why is Breast Screening Important?
Breast cancer screening is crucial as cancerous growth can be detected before physical lumps are felt and seen on the breasts. It allows for early detection and appropriate treatments can be done.
Risk Factors for Breast Cancer
“Risk factors” are anything that increases your risk of developing breast cancer and they can be classified as “modifiable risk factors” and “non-modifiable risk factors”.
Modifiable Risk Factors
- Weight: Keeping to a healthy weight lowers your risk of breast cancer
- Diet: Adopt healthy eating habits with a balanced diet, avoid processed foods
- Alcohol Consumption: Limit your alcohol intake
- Hormone Replacement Therapy (HRT): Being on HRT for prolonged periods of time
Non-modifiable Risk Factors
- Age: Women aged 50 and above
- Family history: If you have a first-degree relative (mother, daughter, sister) who has had breast cancer, or multiple relatives affected by breast or ovarian cancer, you could be at higher risk of getting breast cancer.
- Early-onset of menstruation or late menopause: Starting menstruation early (before the age of 12) and going through menopause late (after age of 55)
What is a Mammogram?
Mammogram is an x-ray image of the breast.
Breast cancer can be detected early with a mammogram for women who have no symptoms or indicators of the disease. This type of mammogram is called a “Screening Mammography”. Two or more x-ray photos, or images, of each breast, are commonly used in screening mammograms. X-ray pictures can often discover malignancies that are not visible to the naked eye. Microcalcifications (small calcium deposits) found on screening mammography can sometimes signal the existence of breast cancer.
After a lump or other sign or symptom of breast cancer has been discovered, mammograms can be performed to check for the illness. This is called a “Diagnostic Mammography”. Diagnostic mammography can also be used to examine alterations discovered during a screening mammogram, or to view breast tissue when obtaining a screening mammogram is not possible due to a variety of factors, such as the existence of breast implants.
According to Singapore’s national guidelines, the recommended age for mammogram screening are:
- Women over the age of 50, who should have a mammogram every two years and
- Women between the ages of 40 and 49, who should have a mammogram once a year.
- Mammogram screening is not required for women under the age of 40, instead a regular breast self-examination (BSE) can be done monthly. Consult your doctor immediately, if you detect any abnormal changes to your breasts seem abnormal.
Difference between Diagnostic and Screening Mammograms
Both types of mammography are performed using the same machine. While a diagnostic mammography takes longer to complete than screening mammography, the overall dosage of radiation is larger since more x-ray images are required to acquire several views of the breast. A worrisome spot may be magnified by the radiology technician to provide a detailed image that can aid the doctor in making an accurate diagnosis.
How is a Mammogram done?
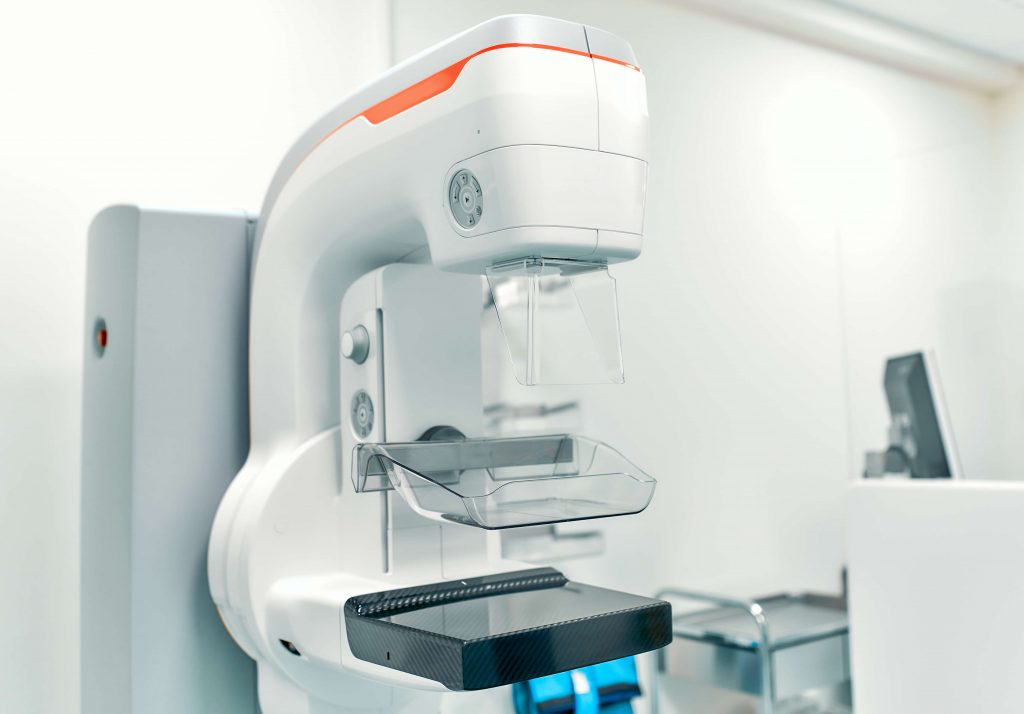
During a mammogram, you will be asked to stand in front of a unique X-ray machine. A radiology technician will guide you through and your breast will be placed on a plastic plate. From above, another plate will firmly squeeze your breast, keeping it in place while the X-ray is taken. You will change positions and the steps are repeated to take a side view of the breast. In the same way, the X-ray will be taken for the other breast.
After the mammogram, you’ll have to wait while the technician examines the four X-rays to ensure they don’t need to be redone. The lab will submit your mammogram report to your doctor.
What does a Mammogram feel like?
Most women may wonder if a Mammogram is painful. As your breast is compressed during a mammogram to obtain clear images, you may expect to feel some discomfort or pain. Should you experience pain during the screening, inform the radiology technician immediately.
It is also advisable to schedule your mammogram 7 to 10 days after the start of your period so your breasts are less tender. You may also opt to take 1 or 2 painkillers before your mammogram, to reduce any potential discomfort or pain.
When will I get the results of my Mammogram?
The results of your mammogram are usually available within a few weeks, after it is reviewed by a radiologist and your healthcare provider. Your doctor will discuss and inform you of your mammogram result: normal or abnormal.
If Mammogram Result is Normal
Do continue with regular mammograms. Doing a comparison of your annual mammogram results are effective in allowing the radiologist and your doctor to see if your breasts have changed. It also helps to keep a record of your medical history.
If Abnormalities Discovered in Mammogram
An abnormal mammogram result does not always indicate the presence of cancer. However, the doctor will need to perform additional mammograms, tests, or exams before he or she can be certain. It does not necessarily imply that you have cancer or that you will require surgery. Doctors will conduct several follow-up tests to determine whether or not there is cancer in the breast, and advise on the appropriate treatment if required.
Conclusion
Even if you feel well, you should go for scheduled mammograms. According to the national guidelines, women above the age of 40 should go for a mammogram once every year, and women above the age of 50 should go for a mammogram once every 2 years.
Early detection through regular screening is critical in fighting breast cancer. When detected early, it enables doctors to offer simpler treatments and achieve better survival outcomes..
At SOG, we provide health screening packages that cover your health & medical needs, and our dedicated team of specialists are ready to help you throughout your journey with us.
🌐 Sign up for SOG Classic Screen with Mammogram Package at: https://www.sog.com.sg/health-screening/classic-screen-with-mammogram/
✅ Classic Screen Package (essential screening tests)
✅ Mammogram (breast cancer screening)
For more information about our health screening packages and the various tests included in our Classic Screen package, visit https://bit.ly/SOGHealthScreening
WHO WE ARE
About SOG Health Pte. Ltd.
Established in 2011, SOG Health Pte. Ltd. (“SOG”) is a leading healthcare service provider dedicated to delivering holistic health and wellness services to the modern family.
With a long and established track record in Singapore providing Obstetrics and Gynaecology (“O&G”) services such as pre-pregnancy counselling, delivery, pregnancy and post-delivery care, the Group has since further expanded its spectrum of healthcare services to include Paediatrics, Dermatology, and Cancer-related General Surgery (Colorectal, Breast & Thyroid).
The Group’s clinics, under its four operating segments of O&G, Paediatrics, Oncology and Dermatology, are strategically located throughout Singapore to provide easy access to its patients.
- Obstetrics
- Gynaecology
- GynaeOncology
- Breast, Thyroid & General Surgery
- Colorectal, Endoscopy & General Surgery
- Dermatology
- Paediatrics
Consult With A Specialist From SOG
Visit one of our specialists today to learn more about your health!
Recommended Specialist
Book An Appointment
Fill up this form and our clinic will get back to you shortly.
For general enquiries, please click here.




