Lifestyle and Beauty
Psoriasis: Causes, Triggers, Diagnosis & Treatment
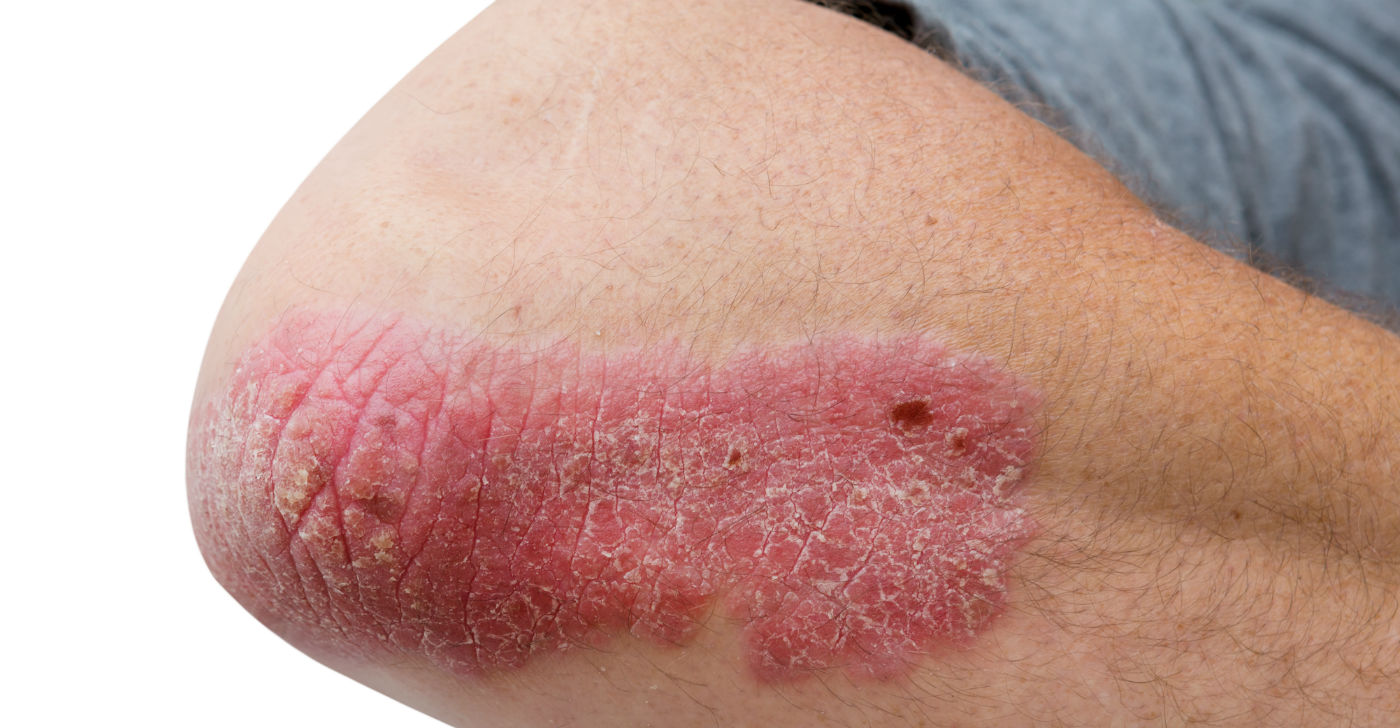
Psoriasis is among the top ten most common skin diseases treated in Singapore, and it is estimated that 1-2% of Singaporeans are diagnosed with psoriasis.
This skin condition more commonly develops between the ages of 15 and 35, but can also develop at any age, equally affecting men and women. It can affect any part of your body but mostly appears as small patches on your knees, scalp, lower back, and elbows.
Symptoms of psoriasis could disappear without apparent reason (go into remission), before flaring up again upon exposure to certain triggers.
What Causes Psoriasis?
The real cause of psoriasis is unknown, but we do know that the immune system and genetics play a significant role in its development. In fact, scientists believe that approximately 10% of people inherit one or more genes that could lead to psoriasis.
Your immune system comprises of a special type of cells known as T cells. The primary function of these cells is to fight viruses, bacteria, and other disease-causing microorganisms. When you have psoriasis and are exposed to triggers, your T cells mistakenly fight healthy skin the same way they fight unwanted viruses and bacteria.
Your immune system responds by sending more blood to the area and producing more white blood cells and skin cells in the affected area. In a normal person, a skin cell cycle lasts between 3 to 4 weeks before being replaced by new cells. However, in people with psoriasis, the same process could take place within days instead of weeks.
With time, the rapid growth of skin cells makes it difficult for them to be shed quickly enough. Newly produced cells move to the outermost layer of the skin too quickly, finally building up at the skin surface as thick, scaly psoriatic patches.
Possible Triggers Of Psoriasis
Psoriasis triggers are not universal. This means that what may trigger psoriasis in one person may not affect another. Some of the possible triggers include:
- Stress: High stress levels may easily trigger a flare-up. If you learn how to relax and manage your stress, you can reduce and possibly prevent potential flare-ups.
- Smoking: Smoking makes it harder to get rid of the symptoms and manage the condition. It is also closely linked with a type of pustular psoriasis that mostly affects your hands and soles of your feet.
- Obesity: Excess weight increases the risk of psoriasis. Lesions associated with all types of psoriasis often develop in your skin creases and folds.
- Infections: Anything that can affect your immune system can easily trigger psoriasis. In particular, strep throat is known to trigger guttate psoriasis in children. Other infectious diseases can cause your body’s immune system to respond, leading to the outbreak of psoriasis.
- Medications: Lithium, which is used to treat bipolar disorder and beta-blockers for high blood pressure, can increase the risk of psoriasis. Various drugs that are used to prevent and treat malaria may also trigger psoriasis.
- Injury to your skin: Psoriasis may develop in areas of your skin that have been traumatized or injured. This is commonly referred to as the Koebner phenomenon. Sunburns, scratches, and vaccinations can trigger a Koebner response as well.
5 Types Of Psoriasis
1) Plaque Psoriasis
This is the most common type of psoriasis, and it causes dry red patches and silvery scales to your skin. These plaques can appear anywhere on your skin, but they often appear on your elbows, knees, scalp, and lower back. They can be painful, and sometimes, they crack and bleed.
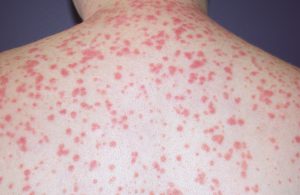
2) Guttate Psoriasis
Guttate psoriasis is common among children, and it usually causes small pink spots. It develops on the torso, arms, and legs. The spots caused by guttate psoriasis are rarely thick or raised like plaque psoriasis.
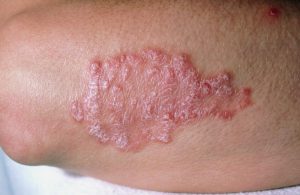
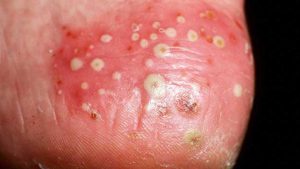
3) Pustular Psoriasis
Pustular psoriasis is usually characterised by relatively large white pustules surrounded by bright red skin. Pustules are relatively large blisters of non-infectious pus. The pus consists of white blood cells and is neither an infection nor contagious. Pustular psoriasis can appear on any part of your body but most often occur on the hands and feet.
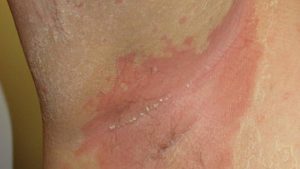
4) Inverse Psoriasis
Inverse psoriasis causes smooth patches of red, inflamed skin that tend to worsen with sweating or friction. Inverse psoriasis mainly affects the skin in the groin, armpits, around the genitals, and under the breasts. Sometimes, fungal infection can trigger this type of psoriasis.
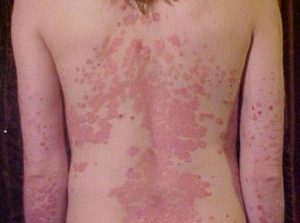
5) Erythrodermic Psoriasis
Erythrodermic psoriasis is rare but aggressive. It can cause a bright red rash that covers your entire body making your skin look as if it has been burned. In most cases, erythrodermic psoriasis is accompanied by intense pain, itching, inability to maintain proper body temperature, and a fast heartbeat.
How Is Psoriasis Diagnosed?
The diagnosis of psoriasis is fairly straightforward. There are no special tools or blood tests required to diagnose the condition. An experienced dermatologist will be able to examine affected skin and determine if the skin disease is psoriasis.
Sometimes, your dermatologist may take a sample of the affected skin and examine it under a microscope to confirm psoriasis. When observed under a microscope, psoriasis skin looks thicker and inflamed compared to skin with eczema.
Your dermatologist may also want to know your family history since research shows that a significant number of people with psoriasis have a close family member with the disease.
Latest Articles
How Are Abdominal Hernias Treated?
What to Expect from Colorectal Surgery
How to Treat Breast Inflammatory Conditions
Gynaecomastia: Understanding Male Breast Cancer
How Is Psoriasis Treated?
If a diagnosis is confirmed, your dermatologist will recommend the most appropriate treatment option depending on the type and severity of your psoriasis.
Your dermatologist may try one therapy and then switch to another, or recommend a combination of several therapies to find out which one works best for you. What works for a time period may even stop being effective, and you may need to switch to another alternative. Therefore, it is recommended that you work closely with your dermatologist to stay on top of your treatment.
Topical Treatments
Comprise of creams, lotions, and ointments that you apply directly to your skin. They include moisturizers, vitamin D creams, and prescription corticosteroids. Shampoos made with coal tar or salicylic acid also fall into this category.
Light Therapy
Light therapy makes use of ultraviolet light or natural light to kill the overactive white blood cells that are attacking your healthy skin cells and causing rapid growth. Phototherapy may be performed in the doctor’s office or at home. Both UVA, and UVB light may help manage symptoms of mild to moderate psoriasis.
Systemic Medications
People with moderate to severe psoriasis and those who have not responded well to other psoriasis treatments may need to use oral or injected medications to manage their condition. Such medication includes retinoids, cyclosporine, methotrexate, and biotics.
Your dermatologist may hesitate to recommend some of these medications which have severe side effects and may be prescribed for a short period only.
Psoriatic Arthritis
5-15% of patients with psoriasis have joint inflammation with mild symptoms of arthritis, commonly referred to as psoriatic arthritis. This condition causes inflammation and progressive damage to your joints. Psoriatic arthritis is common among psoriatic adults who are between 30-50 years old.
Conclusion
Psoriasis is a skin condition that accelerates the growth of skin cells. The disease causes skin cells to build up rapidly on the surface of your skin, leading to the formation of red patches or scales that can sometimes be itchy and painful. Potential triggers of psoriasis include infections, stress, alcohol, smoking, certain medications, and skin injury.
If you suspect you have developed psoriasis, make sure that you see an experienced dermatologist who will diagnose your skin condition and recommend an appropriate treatment method.
WHO WE ARE
About SOG Health Pte. Ltd.
Established in 2011, SOG Health Pte. Ltd. (“SOG”) is a leading healthcare service provider dedicated to delivering holistic health and wellness services to the modern family.
With a long and established track record in Singapore providing Obstetrics and Gynaecology (“O&G”) services such as pre-pregnancy counselling, delivery, pregnancy and post-delivery care, the Group has since further expanded its spectrum of healthcare services to include Paediatrics, Dermatology, and Cancer-related General Surgery (Colorectal, Breast & Thyroid).
The Group’s clinics, under its four operating segments of O&G, Paediatrics, Oncology and Dermatology, are strategically located throughout Singapore to provide easy access to its patients.
- Obstetrics
- Gynaecology
- GynaeOncology
- Breast, Thyroid & General Surgery
- Colorectal, Endoscopy & General Surgery
- Dermatology
- Paediatrics
Consult With A Specialist From SOG
Visit one of our specialists today to learn more about your health!
Recommended Dermatologists
Book An Appointment
Fill up this form and our clinic will get back to you shortly.
For general enquiries, please click here.